Fascias, microbiota and muscle pain: what your belly tells your muscles
Back pain, knees, tendons... What if the solution wasn't just where you're hurting? More and more research shows that chronic muscle and joint pain are often related to much deeper imbalances, which involve an unknown tissue called fascia, but also... Your intestine. Here's what science says about these surprising connections — and how to act in practice.
The human body: a global system, not a sum of spare parts
For a long time, muscle and joint pain have tended to be treated very localized: we treat the knee that hurts, we operate the disc that degenerates, we massage the tendon that pulls. This approach is useful but incomplete.
Chronic pain — i.e. those which last several weeks or months — are not the simple result of a damaged structure. They are often the local expression of a global imbalance that affects the whole body. Three actors play a central role in this mechanism: the immune system, fascia, and intestinal microbiota. These three systems interact constantly, and when one malfunctions, others suffer.
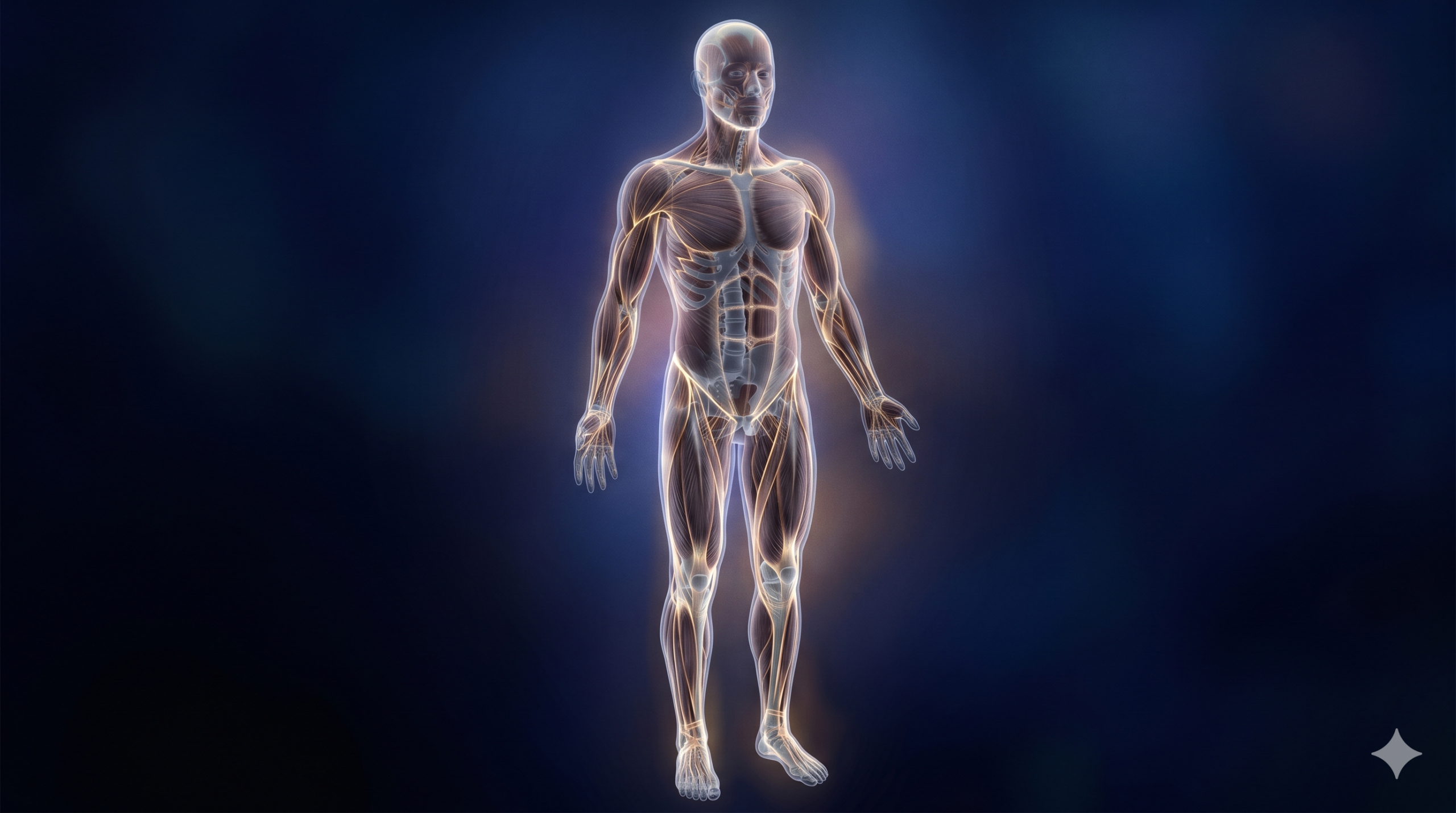
Fascias: the fabric everyone forgets
What is a fascia?
Imagine an inner combination that would wrap every muscle, every bone, every organ, every nerve of your body, from feet to head, continuously and continuously. That's exactly what fascia are. This fibrous tissue, mainly composed of collagen, forms an uninterrupted network in the whole body. In an adult of 80 kg, fascia represent about a quarter of the body mass — or about 20 kilograms.
Fascias are not simple « packaging » liabilities. They play several fundamental roles:
– Transmission of forces : when a muscle contractes, the fascia spread this force throughout the body, allowing fluid and coordinated movements.
– Mechanical communication The cells inside the fascia (fibroblasts) capture tensions and transform them into chemical signals, as a kind of secondary nervous system.
– Immunomodulation Fascias secrete substances that attract or restrain immune cells.
– Perception of pain Fascias are extremely rich in pain receptors. They contain the highest concentration of nerve endings free from the whole organism.
– Slide of layers : Each fascial layer is separated by hyaluronic acid (the same substance used in aesthetic medicine) which allows the structures to slide over one another.
When the fascia get painful
Stress, lack of activity, injury, repeated mechanical overload or inflammation can affect fascia. They then become more rigid, lose their slipping capacity, and ignite. Analyses of painful fascia revealed the presence of many inflammatory mediators, which confirms that fascia itself is often the main source of chronic pain. — and not just the structure it surrounds (tendon, disc, cartilage).
Concrete example : In tendinopathy (inflammation of tendons), the pain comes mainly from the paratenon — the fascia that wraps the tendon — And not the tendon itself. Studies have shown that 34% of asymptomatic tendons have internal degenerations. In other words, the tendon can be damaged without hurting, because it is the fascia around it that is inflamed and innerved.
This same principle applies to lumbar pain (thoraco-lumbar fascia), osteoarthritis (articular capsule, which is a specialized fascia), and diffuse muscle pains such as fibromyalgia.
Chronic inflammation: the silent motor of pain
To understand why fascia are burning, we need to talk about inflammation. Inflammation is a normal and useful response of the body to injury or infection. The problem occurs when this inflammation becomes Chronic , i.e., persistent and low intensity, as a fire that constantly incubates in the body.
This chronic inflammation is orchestrated by chemical messengers called cytokines (in particular, IL-1β, TNF-α and IL-6). These molecules degrade tissues, damage collagen, activate immune cells and maintain pain. What the researchers have discovered is that these same cytokines are present in all chronic musculoskeletal pathologies, whether it be arthrosis, back pain, tendinopathy or fibromyalgia. — as if all these diseases share the same basic mechanism.
Another aggravating factor is what is called the mechanical-inflammatory cycle: structural failure (bad posture, overload, injury) creates stress on fascia, which simmers, which further weakens structures, creating new stress... And so on. This self-sustaining cycle explains why these pains tend to last and worsen over time.
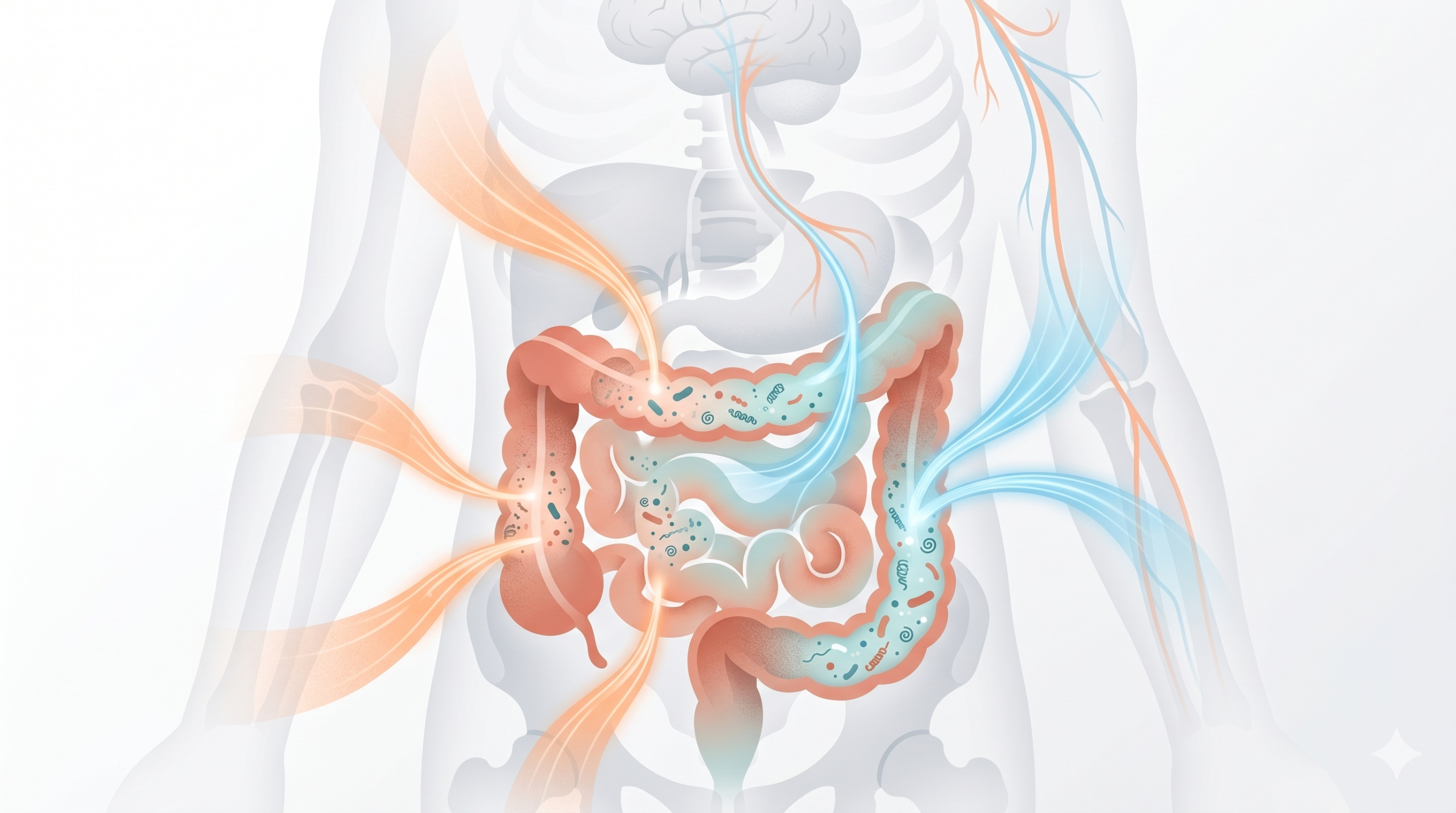
The intestinal microbiota: your intestine controls your inflammation
The intestine, much more than a digestive organ
Your intestine is home to about 38,000 billion micro-organisms (bacteria, fungi, viruses, etc.) that form what we call the intestinal microbiota. This ecosystem plays a key role in digestion, immunity, vitamin production... but also, and this is what we are interested in here, in the regulation of inflammation at the scale of the whole organism.
When the microbiota is balanced and diversified, it helps maintain a good intestinal barrier (the intestine only lets pass what it takes) and keeps inflammation at a normal level.
Dysbiosis: when intestinal flora derails
We're talking about dysbiosis when the balance of the microbiota is disturbed: the good bacteria (like the Bifidobacterium and Akkermansia) decrease, and pro-inflammatory bacteria increase. This situation can occur because of many factors: a low fibre diet, chronic stress, lack of sleep, taking antibiotics, sedentarity...
When dysbiosis settles, the intestinal wall may become too permeable — This is what we call the leaky gut or « permeable intestine ». Fragments of bacteria (including LPS, a bacterial toxin) then pass into the bloodstream, causing persistent systemic inflammation.
The intestinal-muscle-joint connection
This inflammation of intestinal origin affects all tissues of the body, including cartilage, vertebral discs, tendons and fascia. Research has even detected bacterial DNA within degenerated vertebral discs and in arthrosic knee cartilage.
Studies on fibromyalgia are even more striking: the simple transfer of the microbiota from fibromyalgic patients to healthy mice was sufficient to cause hypersensitivity to pain in the latter. Evidence that the microbiota is not just a passenger of the disease, but one of its actors.
What it makes for your health
Treat the cause, not just the symptom
This paradigm calls into question the purely local approach to pain. Treating only the painful structure (operation of a disc, infiltrating a tendon) without dealing with systemic inflammation or surrounding fascia often gives disappointing results in the long term.
A more comprehensive approach integrates several levels of action simultaneously.
1. Acting on food and microbiota
Some foods and supplements have demonstrated their ability to reduce inflammation and restore intestinal balance:
– Omega-3 (EPA and DHA) : present in fatty fish (salmon, sardines, mackerel), they powerfully restrain the inflammatory mechanisms. A dose of 2 to 3 g per day is recommended in a therapeutic context.
– Curcumin (curcuma) : blocks several routes of inflammation at the same time. Its absorption is increased in combination with piperine (black pepper).
– Probiotics and prebiotics : probiotics (fermented yogurt, kefir, sauerkraut...) reintroduce good bacteria. Prebiotics (artichoke fibres, garlic, leeks, bananas...) feed them. Together, they strengthen the intestinal barrier and reduce circulating toxins.
– Fermentable fibres They produce short chain fatty acids (including butyrate) that have a direct anti-inflammatory effect on the intestinal and systemic levels.
– Glutamine, zinc and vitamin D : essential nutrients to repair and maintain the integrity of the intestinal wall.
2. Care for the fascia
Fascias respond very well to targeted interventions:
– Regular movement is the best friend of the fascia. Prolonged immobility is one of their worst enemies: it promotes stiffness and grip.
– Manual therapies (chiropractia, physiotherapy, facial massage, soft stretching) allow to release the areas of tension and restore the slip between the layers.
– Stretching and mobility exercises (yoga, Pilates, dynamic stretching) maintain the elasticity of fascia.
– Moisture is also crucial: fascia need water to maintain their fluidity.
3. Adopt a well calibrated physical load
Regular physical exercise is one of the most powerful anti-inflammatory levers ever. Moderate endurance sessions (fast walking, cycling, swimming, light racing) reduce levels of inflammatory cytokines over the long term. An ideal program includes 3 to 5 cardio activity sessions per week, combined with 2 overall muscle building sessions.
However, overtraining can have the opposite effect and maintain inflammation. Gradual progression and respect for body signals are essential.
4. Managing stress and sleep
Chronic stress activates inflammation mechanisms in white blood cells, resulting in an increase in pro-inflammatory cytokines. Conversely, stress management techniques such as cardiac consistency (breathing 5 seconds of inspiration / 5 seconds of exhalation), meditation or slow breathing activate the vague nerve, which has a naturally anti-inflammatory effect.
Sleep plays an equally important role: a lack of sleep significantly increases inflammatory markers in the blood. Targeting 7 to 9 hours of regular sleep is a health strategy in its own right.
5. The role of collagen
Collagen is the structural protein of fascia, tendons, cartilages and bones. Hydrolysed collagen supplementation (especially as specific peptides) has shown positive results in certain pathologies: improvement of tendinous structure, reduction of joint pain in mild to moderate forms of osteoarthritis.
An important shade: collagen is beneficial only in an anti-inflammatory context. If inflammation is still very active, it is better to control it first before introducing this supplementation. Vitamin C is also essential in combination, as it is the essential cofactor for the manufacture of mature collagen by the body.

What to remember: a global vision of pain
Chronic muscle, joint and tendinous pain is not a fatality, nor a mere consequence of age or wear. They are often a sign of a systemic imbalance that can be addressed at several levels.
The three pillars of this integrative approach are:
1. The intestine : an unbalanced microbiota generates a background inflammation that spreads throughout the body and reaches muscles, joints and fascia.
2. The fascia This often neglected tissue is both a path of pain amplification and a major therapeutic target. Release, mobilize and maintain fascia can relieve pain where other treatments have failed.
3. Inflammation It is at the heart of all these pathologies and can be modified naturally thanks to diet, exercise, sleep and stress management.
Take care of your intestine, move regularly, sleep well, manage stress and eat anti-inflammatoryly: these levers seem simple — And they are. But their combined impact on musculoskeletal health is now supported by sound scientific evidence. This is the future of chronic pain management: a medicine that treats the human being in its entirety, rather than organ by organ.
This article was written for educational and informative purposes. It does not replace a medical opinion. If you have chronic pain, consult a healthcare professional.
__________________________
@Lonhea – Patented Method


